荣格工业资源APP
了解工业圈,从荣格工业资源APP开始。
寻常痤疮是一种多因素共同影响的持续的慢性皮脂腺毛囊皮肤炎症疾病,青少年和年轻人是高发人群[1]。青春期前的儿童也会发生痤疮,分为婴儿痤疮、儿童期痤疮和青春期前痤疮。青春期前痤疮指的是7-12岁的儿童发生的痤疮,这个年龄段的痤疮可能是正常的生长发育的一部分,但有时也可能是内分泌失调的标志[2,3]。
Eichenfield等人的调查发现,青春期前痤疮并不罕见,在近10年增长很快[4]。并且可能是因为青春期的提前,在6-7岁的儿童中越来越多的出现痤疮初期症状[5,6]。Park等人的一项基于社区的横断面研究[7]显示,在693名参与研究的儿童(7-12岁)中,36.2%被诊断患有痤疮,患病率随着年龄的增长而增加。
由于青春期前痤疮患者年龄较低,加之青少年可能对自己的外表缺乏安全感,容易受到同伴意见的影响[2],更需要早期预防和治疗,以防止痤疮在青春期的恶化、疤痕形成[8]和造成心理负担[9–11]。
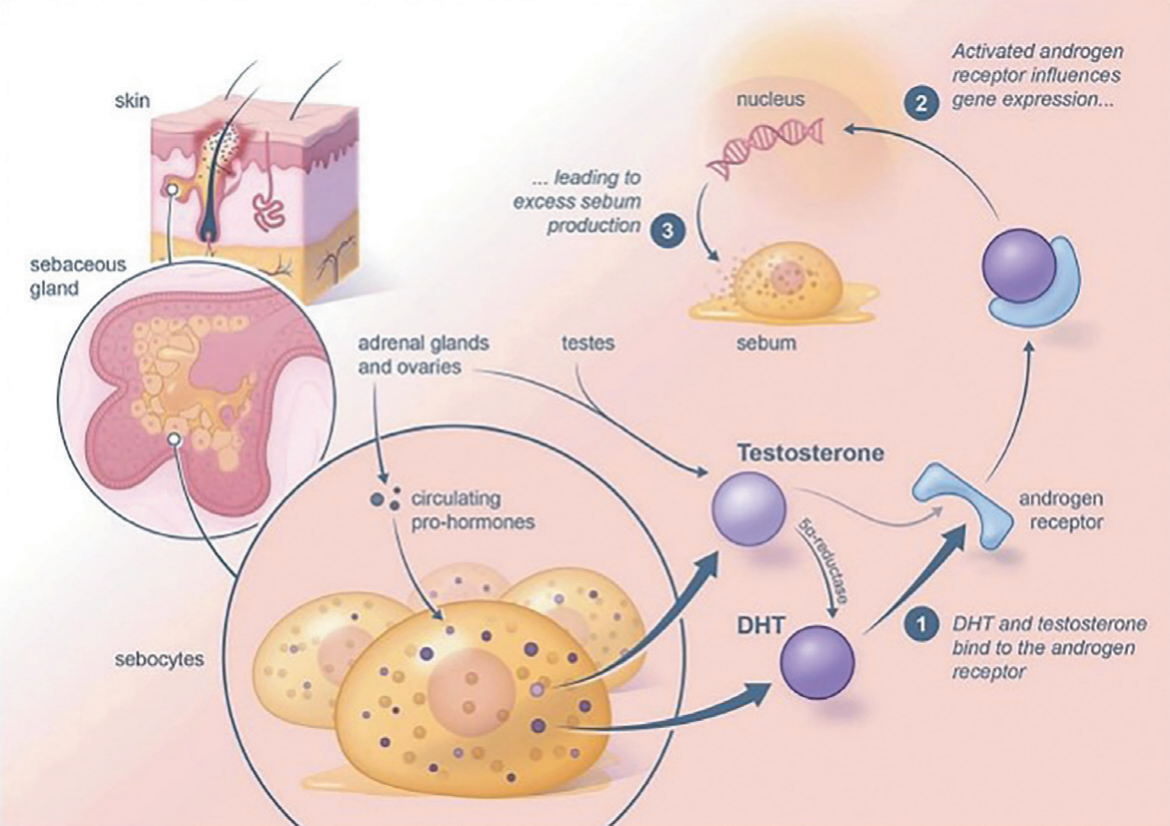
图 1. 雄性激素在痤疮病理生理学中的作用[4]。循环激素(Circulating pro-hormones)由肾上腺、睾丸和卵巢产生,可在皮脂腺内转化为睾酮和二氢睾酮。皮脂细胞表达5α-还原酶,将睾酮转化为更有效的二氢睾酮。二氢睾酮和睾酮结合到皮脂细胞内的雄激素受体,使其转移到细胞核并作为转录因子导致痤疮中的皮脂分泌过多,从而导致炎症,影响角质细胞的增殖和分化,导致毛囊角化过度。
青春期前痤疮的病理生理学
激素变化引起的脂质分泌增加
青春期早期的激素变化是青春期前痤疮的主要影响因素。雄激素是影响皮脂产生的主要因素,而皮脂分泌过度又会导致痤疮[12]。其中二氢睾酮(DHT)是最常见的参与痤疮发展的雄激素之一。DHT与皮脂细胞内的雄激素受体结合,使其转移到细胞核并作为转录因子导致痤疮中皮脂分泌过多[4](图1)。过度分泌的皮脂(如角鲨烯和甘油三酯等)又会导致炎症和痤疮丙酸杆菌增殖,同时影响角质细胞的增殖和分化导致毛囊过度角化[13–18]。而脱氢表雄酮(一种雄激素)水平可能是引起粉刺的重要因素[19]。
毛囊皮脂腺角化过度
皮脂腺角化过度是引起粉刺的重要因素之一。粉刺和丘疹是青春期前痤疮的各种临床表现中最常见的病变[20,21]。对于青春期前患有痤疮的儿童,随着激素和皮脂组成改变,局部细胞因子产生和细菌的异常都与皮脂腺角化过度有关[22]。Oulès等人的研究[23]显示,正常人皮肤的上毛囊皮脂腺单位中表达的GATA6(一种编码转录因子的基因)在痤疮中下调。由于GATA6控制角质细胞的增殖和分化以防止皮脂腺漏斗部角化过度,所以GATA6可能成为减少和预防粉刺的新靶点。
微生态失调与痤疮丙酸杆菌
在于人体皮肤表面的大量微生物,与维持皮肤屏障功能息息相关[24,25]。皮肤微生物菌群之间的平衡对于维持皮肤稳态和控制炎症非常重要[25]。Ahluwalia等人的一项针对7-12岁青春期前儿童皮肤微生物组研究[26]中发现,随着病变(皮损、粉刺等)数量的增加Streptococcus mitis的丰度呈下降趋势,而C.acnes的丰度呈上升趋势。并且粉刺部位提取的C.acnes丰度高于面部其他部位(脸颊、额头、鼻子和下巴)。虽然青春期前痤疮存在皮肤微生物组成的改变,但是在健康人的皮肤上C.ances对皮肤屏障功能起着积极的作用[27]。
Dréno等人的研究[28]表明,痤疮患者皮肤微生物组与健康人的差异是C.acnes系统内的菌群失调。C.acnes菌株分为六种系统型IA1、IA2、IB、IC、II和III [29]。其中,IA1型占主导地位是炎症性痤疮患者的主要特证,而II型在健康人群中更普遍[17,25,28,30]。多项研究显示IA1型产生生物膜和毒力因子的能力更强[31–37],使得针对IA1型菌株的靶向治疗手段可能会成为治疗痤疮的新策略。
免疫反应和炎症
炎症在痤疮的发病机制中起着核心作用。在炎症过程中,先天免疫系统和适应性免疫系统协同激活,诱导免疫反应[38]。痤疮早期存在许多临床上不明显的粉刺和炎症病变的前兆被称为微粉刺[22]。微粉刺中包含大量脂质、C.acnes和脂肪酶[39]。Huang等人阐述了微粉刺在早期痤疮炎症中的影响[38]。
微粉刺带来的毛囊微环境的改变会刺激皮肤驻留的抗原呈递细胞(APC)、皮脂腺细胞和角质形成细胞产生促的炎细胞因子(如 IL-1β、IL-6 和 TGF-β);随后是肥大细胞、先天淋巴样细胞和Th细胞表达产生多种促炎细胞因子;随着Th17/Treg 平衡的偏移会导致炎症过程的启动,并对毛囊皮脂腺单位的平衡产生负面影响,破坏毛囊基底的稳定性,最终导致毛囊壁破裂,中性粒细胞接管毛囊,后期 IL-17 增加并快速引发炎症反应。所以有针对性的控制微粉刺中的早期炎症,可能在防止青春期前痤疮发展成为炎症性痤疮中,发挥着重要作用。
青春期前痤疮的治疗
痤疮的治疗一般是局部或全身的维甲酸、抗生素和激素治疗,也包含一些物理治疗手段[40,41]。而大多数痤疮治疗药物的临床试验是在12岁以上的患者中进行的[2]。此外,虽然青春期前痤疮患儿的皮脂量高于健康儿童,但是青春期前痤疮患儿的皮脂量少于成年痤疮患者,这往往会导致他们的皮肤对药物更加敏感[42]。
目前对于青春期前儿童(<12岁)可使用的维甲酸类药物包括:美国FDA批准0.05%维甲酸凝胶用于10岁以上的儿童;0.1%阿达帕林和2.5%过氧化苯甲酰凝胶适用于9岁及以上的儿童[2],其中阿达帕林对于痤疮早期的微粉刺是有效的[43];第四代类维甲酸药物曲法罗汀(Trifarotene)适用于9岁以上儿童,作为一种选择性视黄酸受体γ(RARγ)激动剂在体外和临床被证明有更好的效果和更好的耐受性[44–46]。青春期本身激素变化带来的皮肤敏感性使得维甲酸类药物在针对12岁以下儿童的使用需要格外注意其带来的副作用,例如使用最低计量减少副作用(皮肤发红、刺激和瘙痒)和通过新型药物输送系统提高耐受性[47,48]。
过氧化苯甲酰(BPO)也是最常见的痤疮治疗成分之一。外用BPO能够溶解粉刺,还有抗菌功效,常与抗生素联合使用,降低抗生素耐药性。对于儿童至青少年痤疮提倡单独使用BPO[11],或与清洁剂(pH~5)和保湿霜联合使用作为辅助治疗,以减少BPO治疗引起屏障受损[2]和微生物多样性下降[26,49]。
Moore等人的一项为期12周的IV期开放试验显示,每日一次外用7.5%的氨苯砜凝胶在青春期前痤疮患者(9-11岁)中安全、有效且耐受性良好[50],已被美国FDA批准用于9岁以上儿童痤疮治疗;另一项调研显示,在所有痤疮就诊中(n=1542)最常用的六种非一线药物(壬二酸、水杨酸、乙醇酸、硫黄、间苯二酚和锌)中,只有硫黄和水杨酸是被于青春期前[51]。
此外,激素疗法用于治疗成人和青少年因雄性激素引起的皮脂分泌过量。对于12岁以下儿童,存在内分泌病理证据才会使用激素,因为激素治疗可能影响低龄儿童的发育[2]。
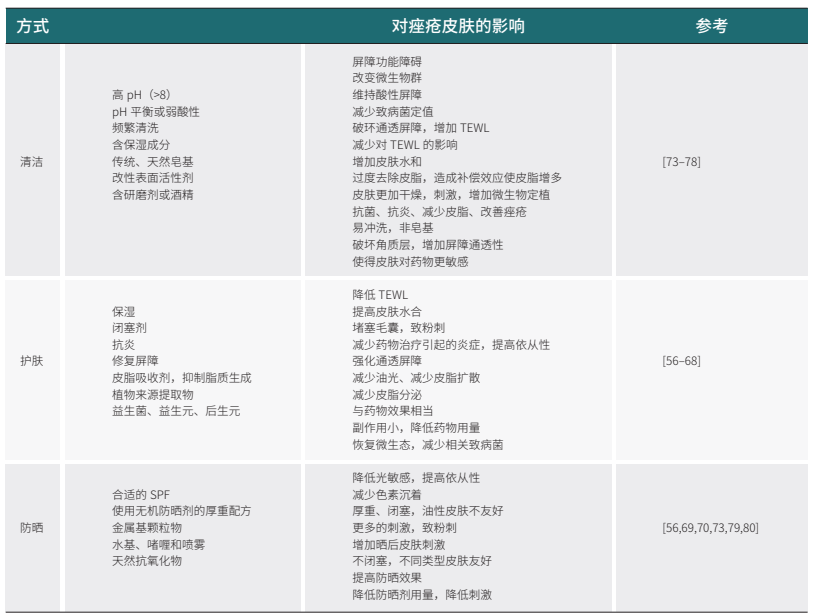
表 1. 清洁、护肤和防晒的重要性
总的来说,对于患有青春期前痤疮的儿童,虽然发病机制与成年人类似,但治疗方法可能因年龄和皮肤成熟度的不同而有所差异,应当尽量使用低剂量、对多种致病因素起效的治疗方案,并结合护肤方案减少屏障受损。
清洁、护肤和防晒的重要性
虽然对于青春期前痤疮治疗的机理和治疗方法都有了很多的进展,但是有效地治疗痤疮仍然是具有挑战性的,特别是青少年对于治疗的依从性比较低[2,52]。由于治疗本身引起的皮肤炎症会影响受试者的依从性,所以配合适当的清洁和护肤品和防晒产品能减少红斑、脱屑和干燥,从而提高患者的依从性和患者满意度[53,54]。
清洁和护肤品包含控油、抗菌、抗炎、抗氧化和角质溶解剂等多种活性成分,对痤疮患者有多方面的益处,并与良好的患者依从性和高满意度相关[55]。由于痤疮固有的角质层渗透性屏障损伤和角质层中游离鞘氨醇和总神经酰胺减少[56],所以使用含有神经酰胺的保湿产品有助减少炎症和干燥,修复通透性屏障,并通过改善药物使用者的皮肤舒适度提高患者的依从性[53]。烟酰胺是维生素B3的一种形式,用于护肤品可以减少皮脂/油脂分泌,防止皮肤产生痤疮[57]。同时烟酰胺具有抗炎特性,治疗轻度至中度痤疮时与BPO联合使用效果好于单独使用BPO[58]。
此外,植物来源的天然提取物在护肤品中非常的常见,也很受欢迎。其中,基于寻常痤疮的临床治疗效果,大多数试验表明,草药可显着减少炎症和非炎症性痤疮病变,并对痤疮严重程度有相关影响[59]。一些药用植物显示出与标准治疗相同或更高的功效[60,61]。植物精油也具有抗炎、抗氧化和抗菌特性,可能对痤疮的多个致病因素有效[62,63]。而具有“宿主微生物选择性利用的基质,具有健康益处”的物质被称为益生元[64]。利用益生元选择性的生物活性恢复微生态平衡的策略也已被应用于痤疮的治疗[65–68]。
除了抗炎、保湿、屏障修复和恢复微生态平衡外,防晒也非常重要。因为一些药物治疗会引起皮肤光敏感[69],导致额外的炎症和色素沉着。此外,UVB(波长在290nm-320nm的紫外线)辐射会增加皮脂腺细胞中的促炎因子的表达,增加角质形成细胞增殖和皮脂生成,UVA(波长在320nm-400nm的紫外线)会增加角质层的厚度,并改变皮肤微生物组,诱发生态失调,可能会加重闭合性粉刺的存在,从而在秋季引起炎症和痤疮发作[70]。可见光(VL)也会加重痤疮炎症后的色素沉着[70]。所以对于患有青春期前痤疮的儿童,建议使用具有良好 UVB 和 UVA 防护的广谱防晒产品以及 VL 防护(遮阳帽和遮阳伞等)。
然而不适当的清洁和护肤可能会引起刺激并加重痤疮,最终影响药物治疗效果[71]。皮脂的减少与痤疮病灶减少显著相关[72],很多青少年会使用更强的清洁产品或频繁地清洗[73]。这反而会进一步破坏皮肤屏障、增加经皮失水、刺激皮肤、增加致病菌定植、引起粉刺、引发性皮炎、灼烧和刺痛等[73,74]。使用pH值较高(>8)的刺激型清洁剂(例如传统的天然皂基)会导致皮肤屏障功能障碍,并改变皮肤和微生物群[75]。这些最终都会导致因无法耐受药物治疗的副作用而降低患者的依从性。而温和且具有屏障保护功能的清洁产品可以在减少皮脂、改善痤疮的同时,降低对屏障的破坏[76–78]。
一些防晒产品会在患者中引起粉刺和痤疮[56,73]。传统的防晒霜成分二氧化钛和氧化锌等金属基颗粒无机化合物的安全性和潜在的毒性的关注越来越多。例如氧化锌纳米颗粒常用与防晒产品,它会加剧UVB暴露后的皮肤损伤[79]。而且无机防晒剂的配方更加厚重且具有闭塞剂,可能引起油性皮肤的皮肤问题[73],这也是防晒导致粉刺和痤疮的一个原因。低SPF值可以减少引发粉刺和痤疮的可能,而天然抗氧化剂在光保护方面的作用有助于提高防晒效果[80],以减少有机防晒剂的用量,降低刺激。
总之,清洁、护肤和防晒对于痤疮皮肤的影响既有积极的方面,也有消极的方面(表1),需要开发合适的痤疮皮肤的配方和推荐正确的清洁和护肤程序。
显然,由于不利和有益两方面的影响,需要更多的研究和仔细观察关于痤疮和皮肤护理的作用,筛选最佳配方特征,以及与局部治疗相结合的方法,以在临床实践领域协助临床医生。通过引入适合的清洁、护肤和防晒方案,提高青春期前痤疮患者的依从性,最终达到最佳治疗效果。
讨论
青春期前痤疮发生在7-12岁的儿童中,并且由于青春期的提前出现低龄化趋势。青春期前痤疮的特点主要是激素变化引起的脂质分泌增加、毛囊皮脂腺角化过度和C.acnes丰度增加,引发粉刺、屏障受损和免疫反应。其中伴随青春期的激素变化是主要影响因素,而这种变化通常与内分泌失调无关[81]。青春期前最常见的症状是粉刺和丘疹,其中粉刺数量显著高于青少年。这个阶段的儿童还有很多痤疮早期阶段的微粉刺和无毛囊壁破坏的小丘疹。由于微粉刺与痤疮早期促炎因子的表达有关,减少已有的微粉刺和预防新的微粉刺形成是可能青春期前痤疮控制的核心。
此外,与健康儿童相比,患有青春期前痤疮的儿童皮肤微生物中,链球菌属丰度降低,丙酸杆菌属丰度增加。虽然成人的研究中表明不是C.acnes丰度增加,而是C.acnes系统内差异,但是在青春期前痤疮患儿中类似的调查有限。Frénard等人针对青春期前痤疮的回顾性研究[8]中同样发现IA1型C.acnes占主导地位,研究对象的平均年龄在17.6 ± 7.5,但是发病年龄在7至12岁。
由于儿童皮肤屏障与成人的存在差异[82],青春期前痤疮治疗需要格外谨慎。而对于低龄化趋势可选择的药物非常有限。虽然这些药物副作用在可接收的范围,但是皮肤发红、刺激、干燥、脱屑,还是会影响患者依从性,从而影响最终治疗效果。
对于青春期前痤疮的治疗,提倡与正确的清洁和护肤作为整体方案,以减少药物剂量和副作用,提高依从性和最终满意度。使用无香料、无刺激性和非致痘的清洁剂、保湿剂和防晒霜可以减少由局部或口服痤疮治疗引起的炎症、干燥、红斑和光敏反应。而不正确的清洁和护肤反而会进一步破坏屏障,导致痤疮加重和治疗的失败。特别是过度清洁和使用有致痘风险的护肤品。
另一个常被忽略的环节是防晒,特别是使用维甲酸或激素治疗的患者,防晒产品可以减少额外的炎症和色素沉着。但是需要特别注意高防晒指数的无机防晒产品可能造成额外的刺激,厚重的配方也可能堵塞毛孔并加重痤疮。而水基、啫喱或凝胶型的含有机防晒剂产品,并且通过抗氧化剂的使用,降低防晒剂用量可能是更加合适的方案。
值得一提的是,Anderson等人的研究[83]表明从一种治疗方法改为几种治疗方法会降低患者的依从性。在导入清洁、护肤和防晒产品作为整体方案时,也应当考虑患者操作的便利性和尽可能的简化步骤。例如将清洁和护肤,或护肤和防晒功效整合在一种产品中。
结论
综上所述,青春期前痤疮需要综合考虑患者的年龄、皮肤类型和痤疮的严重程度,格外谨慎的使用药物,尽量采用低剂量、多种致病途径有效的联合治疗。并且推荐配合正确的清洁,护肤和防晒程序,缓解药物副作用、提高皮肤耐受性,并辅助痤疮治疗,最终提高患者依从性和治疗满意度,这是预防和治疗青春期前痤疮的重要组成部分。
参考文献
[1] Walsh T R, Efthimiou J, Dréno B. Systematic review of antibiotic resistance in acne: an increasing topical and oral threat[J]. The Lancet Infectious Diseases, 2016, 16(3): e23-e33.
[2] Eichenfield L F, Krakowski A C, Piggott C, 等. Evidence-based recommendations for the diagnosis and treatment of pediatric acne[J]. Pediatrics, 2013, 131 Suppl 3: S163-186.
[3] Schachner L A, Eichenfield L, Andriessen A, 等. Consensus on Neonatal Through Preadolescent Acne[J]. Journal of drugs in dermatology: JDD, 2020, 19(6): 592-600.
[4] Eichenfield L, Hebert A, Desai S R, 等. The New Face of Preadolescent and Adolescent Acne: Beyond the Guidelines[J]. The Journal of Family Practice, 2022, 71(6 Suppl): S63-S70.
[5] Bree A F, Siegfried E C. Acne Vulgaris in Preadolescent Children: Recommendations for Evaluation[J]. Pediatric Dermatology, 2014, 31(1): 27-32.
[6] Mouritsen A, Aksglaede L, Sørensen K, et al. Hypothesis: exposure to endocrine‐disrupting chemicals may interfere with timing of puberty[J]. International Journal of Andrology, 2010, 33(2): 346-359.
[7] Park S Y, Kwon H H, Min S, 等. Epidemiology and risk factors of childhood acne in Korea: a cross‐sectional community based study[J]. Clinical and Experimental Dermatology, 2015, 40(8): 844-850.
[8] Frénard C, Mansouri S, Corvec S, 等. Prepubertal acne: A retrospective study[J]. International Journal of Women’s Dermatology, 2021, 7(4): 482-485.
[9] W. Lucky A. A Review of Infantile and PediatricAcne[J]. Dermatology, 1998, 196(1): 95-97.
[10] Niemeier V, Kupfer J, Gieler U. Acne vulgaris--psychosomatic aspects[J]. Journal der Deutschen Dermatologischen Gesellschaft = Journal of the German Society of Dermatology: JDDG, 2006, 4(12): 1027-1036.
[11] Schnopp C, Mempel M. Acne vulgaris in children and adolescents[J]. Minerva Pediatrica, 2011, 63(4): 293-304.
[12] Bharti S, Vadlamudi H C. A strategic review on the involvement of receptors, transcription factors and hormones in acne pathogenesis[J]. Journal of Receptors and Signal Transduction, 2021, 41(2): 105-116.
[13] Ottaviani M, Alestas T, Flori E, 等. Peroxidated Squalene Induces the Production of Inflammatory Mediators in HaCaT Keratinocytes: A Possible Role in Acne Vulgaris[J]. Journal of Investigative Dermatology, 2006, 126(11): 2430-2437.
[14] Chiba K, Yoshizawa K, Makino I, 等. Comedogenicity of Squalene Monohydroperoxide in the Skin After Topical Application[J]. The Journal of Toxicological Sciences, 2000, 25(2): 77-83.
[15] Do T H, Ma F, Andrade P R, 等. TREM2 macrophages induced by human lipids drive inflammation in acne lesions[J]. Science immunology, 2022, 7(73): eabo2787.
[16] Sanford J A, O’Neill A M, Zouboulis C C, 等. Short-chain fatty acids from Cutibacterium acnes activate both a canonical and epigenetic inflammatory response in human sebocytes[J]. Journal of immunology (Baltimore, Md. : 1950), 2019, 202(6): 1767-1776.
[17] O’Neill A M, Gallo R L. Host-microbiome interactions and recent progress into understanding the biology of acne vulgaris[J]. Microbiome, 2018, 6(1): 177.
[18] Kim J. Review of the Innate Immune Response in Acne vulgaris: Activation of Toll-Like Receptor 2 in Acne Triggers Inflammatory Cytokine Responses[J]. Dermatology, 2005, 211(3): 193-198.
[19] Lucky A W, Biro F M, Huster G A, 等. Acne Vulgaris in Premenarchal Girls: An Early Sign of Puberty Associated With Rising Levels of Dehydroepiandrosterone[J]. Archives of Dermatology, 1994, 130(3): 308-314.
[20] Coughlin C C, Swink S M, Horwinski J, 等. The preadolescent acne microbiome: A prospective, randomized, pilot study investigating characterization and effects of acne therapy[J]. Pediatric Dermatology, 2017, 34(6): 661-664.
[21] Pareek V, Khunger N, Sharma S, 等. An Observational Study of Clinical, Metabolic and Hormonal Profile of Pediatric Acne[J]. Indian Journal of Dermatology, 2022, 67(6): 645-650.
[22] Cunliffe W J, Holland D B, Jeremy A. Comedone formation: Etiology, clinical presentation, and treatment[J]. Clinics in Dermatology, 2004, 22(5): 367-374.
[23] Oulès B, Philippeos C, Segal J, et al. Contribution of GATA6 to homeostasis of the human upper pilosebaceous unit and acne pathogenesis[J]. Nature Communications, 2020, 11(1): 5067.
[24] Harris-Tryon T A, Grice E A. Microbiota and maintenance of skin barrier function[J]. Science, 2022, 376(6596): 940-945.
[25] Dagnelie M-A, Montassier E, Khammari A, 等. Inflammatory skin is associated with changes in the skin microbiota composition on the back of severe acne patients[J]. Experimental Dermatology, 2019, 28(8): 961-967.
[26] Ahluwalia J, Borok J, Haddock E S, et al. The microbiome in preadolescent acne: Assessment and prospective analysis of the influence of benzoyl peroxide[J]. Pediatric Dermatology, 2019, 36(2): 200-206.
[27] Fournière M, Latire T, Souak D, 等. Staphylococcus epidermidis and Cutibacterium acnes: Two Major Sentinels of Skin Microbiota and the Influence of Cosmetics[J]. Microorganisms, 2020, 8(11): 1752.
[28] Dréno B, Dagnelie M A, Khammari A, et al. The Skin Microbiome: A New Actor in Inflammatory Acne[J]. American Journal of Clinical Dermatology, 2020, 21(1): 18-24.
[29] Kilian M, Scholz C F P, Lomholt H B. Multilocus Sequence Typing and Phylogenetic Analysis of Propionibacterium acnes[J]. Journal of Clinical Microbiology, 2020, 50(4): 1158-1165.
[30] Dagnelie M-A, Corvec S, Saint-Jean M, et al. Decrease in Diversity of Propionibacterium acnes Phylotypes in Patients with Severe Acne on the Back[J]. Acta Dermato-Venereologica, 2018, 98(2): 262-267.
[31] Coenye T, Spittaels K-J, Achermann Y. The role of biofilm formation in the pathogenesis and antimicrobial susceptibility of Cutibacterium acnes[J]. Biofilm, 2022, 4: 100063.
[32] Barnard E, Johnson T, Ngo T, 等. Porphyrin Production and Regulation in Cutaneous Propionibacteria[J]. mSphere, 2020, 5(1): e00793-19.
[33] Johnson T, Kang D, Barnard E, 等. Strain-Level Differences in Porphyrin Production and Regulation in Propionibacterium acnes Elucidate Disease Associations[J]. mSphere, 2016, 1(1): e00023-15.
[34] Pappas A, Johnsen S, Liu J-C, 等. Sebum analysis of individuals with and without acne[J]. Dermato-endocrinology, 2009, 1(3): 157-161.
[35] Mias C, Mengeaud V, Bessou-Touya S, 等. Recent advances in understanding inflammatory acne: Deciphering the relationship between Cutibacterium acnes and Th17 inflammatory pathway[J]. Journal of the European Academy of Dermatology and Venereology: JEADV, 2023, 37 Suppl 2: 3-11.
[36] Agak G W, Kao S, Ouyang K, et al. Phenotype and Antimicrobial Activity of Th17 Cells Induced by Propionibacterium acnes Strains Associated with Healthy and Acne Skin[J]. Journal of Investigative Dermatology, 2018, 138(2): 316-324.
[37] Spittaels K-J, Van Uytfanghe K, Zouboulis C C, 等. Porphyrins produced by acneic Cutibacterium acnes strains activate the inflammasome by inducing K+ leakage[J]. iScience, 2021, 24(6): 102575.
[38] Huang L, Yang S, Yu X, 等. Association of different cell types and inflammation in early acne vulgaris[J]. Frontiers in Immunology, 2024, 15: 1275269.
[39] Josse G, Mias C, Le Digabel J, 等. High bacterial colonization and lipase activity in microcomedones[J]. Experimental Dermatology, 2020, 29(2): 168-176.
[40] Fox L, Csongradi C, Aucamp M, et al. Treatment Modalities for Acne[J]. Molecules, 2016, 21(8): 1063.
[41] Vasam M, Korutla S, Bohara R A. Acne vulgaris: A review of the pathophysiology, treatment, and recent nanotechnology based advances[J]. Biochemistry and Biophysics Reports, 2023, 36: 101578.
[42] Friedlander S F, Baldwin H E, Mancini A J, et al. The Acne Continuum: An Age-Based Approach to Therapy[J]. Seminars in Cutaneous Medicine and Surgery, 2011, 30(3): S6-S11.
[43] Thielitz A, Sidou F, Gollnick H. Control of microcomedone formation throughout a maintenance treatment with adapalene gel, 0.1%[J]. Journal of the European Academy of Dermatology and Venereology: JEADV, 2007, 21(6): 747-753.
[44] Aubert J, Piwnica D, Bertino B, 等. Nonclinical and human pharmacology of the potent and selective topical retinoic acid receptor-γ agonist trifarotene[J]. The British Journal of Dermatology, 2018, 179(2): 442-456.
[45] Tan J, Thiboutot D, Popp G, 等. Randomized phase 3 evaluation of trifarotene 50 μg/g cream treatment of moderate facial and truncal acne[J]. Journal of the American Academy of Dermatology, 2019, 80(6): 1691-1699.
[46] Eichenfield L, Kwong P, Lee S, 等. Advances in Topical Management of Adolescent Facial and Truncal Acne: A Phase 3 Pooled Analysis of Safety and Efficacy of Trifarotene 0.005% Cream[J]. Journal of Drugs in Dermatology, 2022, 21(6): 582-586.
[47] Eichenfield L F, Sugarman J L, Guenin E, et al. Novel tretinoin 0.05% lotion for the once-daily treatment of moderate-to-severe acne vulgaris in a preadolescent population[J]. Pediatric Dermatology, 2019, 36(2): 193-199.
[48] Eichenfield L F, Hebert A A, Schachner L, 等. Tretinoin microsphere gel 0.04% pump for treating acne vulgaris in preadolescents: a randomized, controlled study[J]. Pediatric Dermatology, 2012, 29(5): 598-604.
[49] Zhou L, Chen L, Liu X, 等. The influence of benzoyl peroxide on skin microbiota and the epidermal barrier for acne vulgaris[J]. Dermatologic Therapy, 2022, 35(3): e15288.
[50] Moore A Y, Lain E L, McMichael A, et al. Once-daily Dapsone 7.5% Gel for the Treatment of Acne Vulgaris in Preadolescent Patients: A Phase IV, Open-label, 12-week Study[J]. The Journal of Clinical and Aesthetic Dermatology, 2021, 14(4): 43.
[51] Afarideh M, Rodriguez Baisi K E, Davis D M R, et al. Trends in utilization of non-first-line topical acne medications among children, adolescents, and adults in the United States, 2012-2016[J]. Pediatric Dermatology, 2021, 38(5): 1066-1073.
[52] Yentzer B A, Alikhan A, Teuschler H, 等. An exploratory study of adherence to topical benzoyl peroxide in patients with acne vulgaris[J]. Journal of the American Academy of Dermatology, 2009, 60(5): 879-880.
[53] Schachner L A, Alexis A F, Andriessen A, 等. Insights into acne and the skin barrier: Optimizing treatment regimens with ceramide-containing skincare[J]. Journal of Cosmetic Dermatology, 2023, 22(11): 2902-2909.
[54] Del Rosso J Q, Gold M, Rueda M J, 等. Efficacy, Safety, and Subject Satisfaction of a Specified Skin Care Regimen to Cleanse, Medicate, Moisturize, and Protect the Skin of Patients Under Treatment for Acne Vulgaris[J]. The Journal of Clinical and Aesthetic Dermatology, 2015, 8(1): 22-30.
[55] Araviiskaia E, Lopez Estebaranz J L, Pincelli C. Dermocosmetics: beneficial adjuncts in the treatment of acne vulgaris[J]. Journal of Dermatological Treatment, 2021, 32(1): 3-10.
[56] Del Rosso J Q, Brandt S. The Role of Skin Care as an Integral Component in the Management of Acne Vulgaris: Part 2: Tolerability and Performance of a Designated Skin Care Regimen Using a Foam Wash and Moisturizer SPF 30 in Patients with Acne Vulgaris Undergoing Active Treatment[J]. The Journal of Clinical and Aesthetic Dermatology, 2013, 6(12): 28-36.
[57] Draelos Z D, Matsubara A, Smiles K. The effect of 2% niacinamide on facial sebum production[J]. Journal of Cosmetic and Laser Therapy, 2006, 8(2): 96-101.
[58] Kaewsanit T, Chakkavittumrong P, Waranuch N. Clinical Comparison of Topical 2.5% Benzoyl Peroxide plus 5% Niacinamide to 2.5% Benzoyl Peroxide Alone in the Treatment of Mild to Moderate Facial Acne Vulgaris[J]. The Journal of Clinical and Aesthetic Dermatology, 2021, 14(6): 35-41.
[59] Kanlayavattanakul M, Lourith N. Therapeutic agents and herbs in topical application for acne treatment[J]. International Journal of Cosmetic Science, 2011, 33(4): 289-297.
[60] Bassett I B, Barnetson R S C, Pannowitz D L. A comparative study of tea‐tree oil versus benzoylperoxide in the treatment of acne[J]. Medical Journal of Australia, 1990, 153(8): 455-458.
[61] Lubtikulthum P, Kamanamool N, Udompataikul M. A comparative study on the effectiveness of herbal extracts vs 2.5% benzoyl peroxide in the treatment of mild to moderate acne vulgaris[J]. Journal of Cosmetic Dermatology, 2019, 18(6): 1767-1775.
[62] Bungau A F, Radu A-F, Bungau S G, 等. Emerging Insights into the Applicability of Essential Oils in the Management of Acne Vulgaris[J]. Molecules (Basel, Switzerland), 2023, 28(17): 6395.
[63] Sitthichai P, Chanpirom S, Maneerat T, 等. Kaempferia parviflora Rhizome Extract as Potential Anti-Acne Ingredient[J]. Molecules (Basel, Switzerland), 2022, 27(14): 4401.
[64] Gibson G R, Hutkins R, Sanders M E, 等. Expert consensus document: The International Scientific Association for Probiotics and Prebiotics (ISAPP) consensus statement on the definition and scope of prebiotics[J]. Nature Reviews. Gastroenterology & Hepatology, 2017, 14(8): 491-502.
[65] Claudel J-P, Auffret N, Leccia M-T, et al. Staphylococcus epidermidis: A Potential New Player in the Physiopathology of Acne?[J]. Dermatology, 2019, 235(4): 287-294.
[66] Wang Y, Kuo S, Shu M, 等. Staphylococcus epidermidis in the human skin microbiome mediates fermentation to inhibit the growth of Propionibacterium acnes: Implications of probiotics in acne vulgaris[J]. Applied microbiology and biotechnology, 2014, 98(1): 411-424.
[67] Cui H, Feng C, Guo C, 等. Development of Novel Topical Anti-Acne Cream Containing Postbiotics for Mild-to-Moderate Acne: An Observational Study to Evaluate Its Efficacy[J]. Indian Journal of Dermatology, 2022, 67(6): 667-673.
[68] Cañellas-Santos M, Rosell-Vives E, Montell L, 等. Anti-Inflammatory and Anti-Quorum Sensing Effect of Camellia sinensis Callus Lysate for Treatment of Acne[J]. Current Issues in Molecular Biology, 2023, 45(5): 3997-4016.
[69] Drucker A M, Rosen C F. Drug-induced photosensitivity: culprit drugs, management and prevention[J]. Drug Safety, 2011, 34(10): 821-837.
[70] Passeron T, Lim H W., Goh C-L, et al. Photoprotection according to skin phototype and dermatoses: practical recommendations from an expert panel[J]. Journal of the European Academy of Dermatology and Venereology, 2021, 35(7): 1460-1469.
[71] Dessinioti C, Antoniou C, Katsambas A. Acneiform eruptions[J]. Clinics in Dermatology, 2014, 32(1): 24-34.
[72] Janiczek-Dolphin N, Cook J, Thiboutot D, 等. Can sebum reduction predict acne outcome?[J]. The British Journal of Dermatology, 2010, 163(4): 683-688.
[73] Goodman G. Cleansing and moisturizing in acne patients[J]. American Journal of Clinical Dermatology, 2009, 10 Suppl 1: 1-6.
[74] Subramanyan K. Role of mild cleansing in the management of patient skin[J]. Dermatologic Therapy, 2004, 17(s1): 26-34.
[75] Li R, Rodrigues M, Li L, 等. Association between skin acid mantle, natural moisturizing factors, and antibacterial activity against s. aureus in the stratum corneum[J]. Clinical, Cosmetic and Investigational Dermatology, 2023, 16: 1595-1606.
[76] Draelos Z D. The effect of a daily facial cleanser for normal to oily skin on the skin barrier of subjects with acne[J]. Cutis, 2006, 78(1 Suppl): 34-40.
[77] Rajaiah Yogesh H, Gajjar T, Patel N, 等. Clinical study to assess efficacy and safety of Purifying Neem Face Wash in prevention and reduction of acne in healthy adults[J]. Journal of Cosmetic Dermatology, 2022, 21(7): 2849-2858.
[78] Mukhopadhyay P. Cleansers and their role in various dermatological disorders[J]. Indian Journal of Dermatology, 2011, 56(1): 2-6.
[79] Wang B-J, Chen Y-Y, Chang H-H, 等. Zinc oxide nanoparticles exacerbate skin epithelial cell damage by upregulating pro-inflammatory cytokines and exosome secretion in M1 macrophages following UVB irradiation-induced skin injury[J]. Particle and Fibre Toxicology, 2024, 21(1): 9.
[80] Dunaway S, Odin R, Zhou L, 等. Natural Antioxidants: Multiple Mechanisms to Protect Skin From Solar Radiation[J]. Frontiers in Pharmacology, 2018, 9: 392.
[81] Mancini A J, Baldwin H E, Eichenfield L F, 等. Acne life cycle: the spectrum of pediatric disease[J]. Pediatric News, 2011, 45(10): S4-S4.
[82] Stamatas G N, Roux P-F, Boireau-Adamezyk E, et al. Skin maturation from birth to 10 years of age: Structure, function, composition and microbiome[J]. Experimental Dermatology, 2023, 32(9): 1420-1429.
[83] Anderson K L, Dothard E H, Huang K E, 等. Frequency of Primary Nonadherence to Acne Treatment[J]. JAMA Dermatology, 2015, 151(6): 623-626.
来源:荣格-《 国际个人护理品生产商情》
原创声明:
本站所有原创内容未经允许,禁止任何网站、微信公众号等平台等机构转载、摘抄,否则荣格工业传媒保留追责权利。任何此前未经允许,已经转载本站原创文章的平台,请立即删除相关文章。

